Mind and Heart:
Understanding Cognitive Changes in Heart Failure
Learn about the experience of cognitive changes in heart failure through the eyes of patients, caregivers, and clinicians.

What is Cognitive Impairment?
Patients with heart failure (HF) are at a greater risk of experiencing cognitive impairment. This can happen due to age, heart failure itself, and other chronic illnesses or risk factors. This contributes to changes in the brain, leading to cognitive impairment.
Cognitive impairment means a change in any or all cognitive elements, such as:
- Memory
- Attention
- Language
- Reasoning
- Concentration
- Executive function (problem solving, decision making, self-regulation of both emotions and behaviour)
Cognitive impairment can range in severity, from mild cases to more severe conditions, such as dementia. A decline in cognitive function may impact the ability to manage medications and appointment schedules as well as communicate symptoms. This decline can also impact everyday quality of life of person with the condition as well as their families and/or caregivers


Heart Failure and Cognition
What can impact Cognitive Impairment in Heart Failure Patients?
CV-related conditions
Hypertension, chronic vascular disease, and atrial fibrillation are risk factors for cognitive impairment.
Non-CV conditions
Diabetes, liver disease, sleep disorders, mood disorders, and chronic kidney disease are also risk factors for cognitive decline in patients with HF.
Factors that may accelerate cognitive decline include:
Medications
Taking multiple medications (known as polypharmacy), to manage one or many conditions, may impact cognitive function. An increased number of medications often means multiple conditions, putting patients at a greater risk of cognitive decline. Some medications, such as sedatives, can impact cognition.
Cardiac surgery
Cardiac surgery can have negative consequences on cognitive function and can lead to delirium. Delirium is a fluctuating confusional state where patients experience an increase in confusion and memory loss, and a decrease in attention.
Heart Failure and Cognition
What is Vascular Cognitive Impairment?
Patients with HF are also at a greater risk of developing vascular cognitive impairment (VCI), which is when there are damaged blood vessels in the brain. This condition can lead to challenges with cognitive abilities. Click through the different stages of diagnoses and their impacts below.
Pre-Diagnosis
Symptoms
Symptoms and Diagnosis
What are the symptoms of Vascular Cognitive Impairment?
Vascular cognitive impairment affects thinking, memory, mood, and daily functioning due to reduced blood flow to the brain. Symptoms can include slowed thinking, difficulty with planning or decision-making, trouble concentrating, memory changes, and challenges with multitasking. People may also notice changes in mood, motivation, walking or balance, and increased fatigue. Symptoms often develop gradually and can vary from person to person, sometimes worsening after a stroke or with ongoing heart and blood vessel disease.
You, or your care partners, may notice:
- Difficulty in managing bills or appointments
- Having a hard time with multitasking
- Losing your train of thought easily
- Forgetting medications or having difficulty recalling names
- Having new problems with following routes
- Challenges with using familiar devices, such as your phone
- Impulsivity, emotional dysregulation, and mood swings
Real Experiences of Cognitive Changes
Symptoms and Diagnosis
Letting Your Clinician Know
Symptoms and Diagnosis
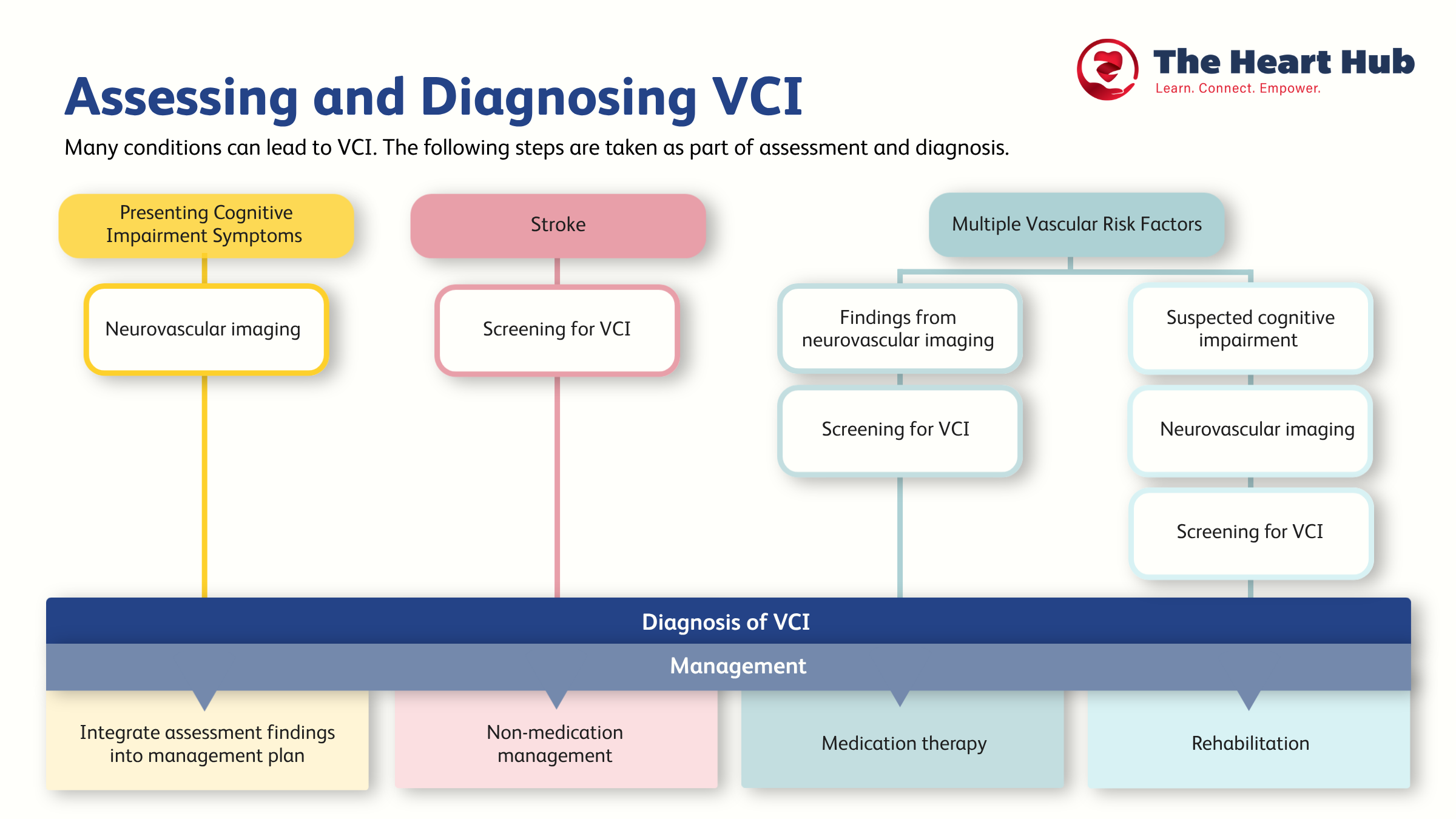
How is Vascular Cognitive Impairment Diagnosed?
The following steps are taken to diagnose vascular cognitive impairment:
1. Comprehensive assessment by a physician leading cognitive testing: Input from the family and/or caregiver is also important to help identify any changes in behaviour or mood.
2. Cognitive testing must be completed: There are several different cognitive tests that can be used, each varying in length of time.
3. Brain imaging should be done so clinicians can assess physical changes in the brain.
See the graphic below to learn more about different pathways to diagnosis and management.
Reducing Risk
Some changes in thinking, memory, or focus can improve when underlying health factors are addressed. Supporting heart health also supports brain health, because the brain depends on steady blood flow, oxygen, and nutrients.
Tips to reduce risk and support reversibility:
- Tell your care team about any changes in memory, attention, or problem solving, even if they feel mild
- Keep blood pressure, blood sugar, and cholesterol within target ranges
- Take medications as prescribed and ask questions if side effects make this hard
- Avoid smoking and limit alcohol
- Stay socially connected, as isolation can worsen cognitive and emotional symptoms
- Address sleep problems, such as poor sleep quality or suspected sleep apnea
Early attention matters. The sooner concerns are raised, the more options there may be to help.
Cognition and Self-Management
Heart failure can affect more than the heart. It can also influence how the brain works, including memory, attention, and thinking speed. The good news is that there are steps you can take to support your brain health.
Managing heart failure through daily self-management such as taking medications as prescribed, staying physically active, eating well, managing stress, and attending regular medical appointments can help maintain healthy blood flow to the brain.
Small, consistent choices can add up over time and may reduce risk while supporting both heart and brain health.
Symptom Management
Tips for managing heart failure symptoms:
- Track daily symptoms such as breathlessness, swelling, weight changes, and fatigue
- Weigh yourself at the same time each day and report sudden changes as instructed
- Pace activities and build in rest periods to avoid extreme fatigue
- Sit upright or use extra pillows if shortness of breath worsens when lying flat
- Report frequent dizziness, light-headedness, or near falls to your care team
- Let your provider know if symptoms are interfering with sleep or daily tasks
Managing symptoms is not just about comfort. It can also help protect thinking and energy levels.
Medical Management
Medical care plays a key role in protecting both heart and brain health. Medications, monitoring, and follow-up visits help keep the heart working more efficiently and reduce strain on the body.
Tips for staying on track medically:
- Keep an up-to-date medication list and bring it to every appointment
- Use a pill organizer or phone reminders to support adherence
- Request blister packs from the pharmacy
- Ask your clinician to explain what each medication is for in plain language
- Do not stop or change medications without medical advice
- Ask about cognitive screening if you are noticing changes in thinking
- Bring a family member or support person to appointments if helpful
If a treatment plan feels confusing or overwhelming, it can and should be adjusted.
Physical Activity
Movement supports circulation, mood, energy, and brain health. Even small amounts of regular activity can make a difference.
Tips for safe physical activity:
- Choose activities that match your current symptoms, such as walking or gentle strength exercises
- Break activity into short sessions if fatigue is a challenge
- Warm up and cool down to reduce strain
- Stop activity if you experience chest pain, dizziness, or severe shortness of breath
- Ask your care team about cardiac rehabilitation or supervised exercise programs
- Focus on consistency rather than intensity
Any movement is better than none, and it should feel achievable and safe.
Diet
Tips for heart and brain supportive eating:
- Aim for meals with vegetables, fruits, whole grains, and healthy fats when possible
- Choose lean proteins such as fish, beans, or poultry
- Follow sodium guidance provided by your care team
- Read food labels to understand sodium content
- Stay hydrated according to your personalized fluid plan
- Ask for a referral to a dietitian if food planning feels overwhelming
Diet does not have to be perfect to be helpful. Small changes can still matter.
Mental Health
Tips to address mental health and stigma:
- Remember that memory or mood changes are health issues, not personal failures
- Talk openly with your clinician about low mood, anxiety, or loss of interest
- Ask about counseling, therapy, or medication options if symptoms persist
- Share concerns with a trusted person rather than carrying them alone
- Notice and challenge negative self-talk when it appears
- Give yourself permission to need support
Seeking help is a sign of strength and self-aware.
- Give permission to a family member or close friend to give honest appraisal of your mood
- Keep a diary of social-emotional thoughts.
Physical Environment
Tips for creating a supportive environment:
- Keep medications in one consistent, visible location
- Use alarms, calendars, or written checklists for daily tasks
- Reduce clutter in frequently used areas
- Store important items like keys, glasses, and devices in the same place
- Post emergency contacts and medication lists in an easy to find spot
- Invite family or caregivers to help set up systems that work for you
The goal is to make daily care easier, not harder.
Introspection and Honesty
Tips for honest self-reflection:
- Notice patterns in symptoms, mood, energy, and memory
- Write down questions or concerns before appointments
- Share what feels hardest, not just what feels manageable
- Be honest about barriers such as cost, fatigue, stress, or forgetfulness
- Ask for help adjusting plans that are not working
- Focus on progress rather than perfection
Clear communication helps turn care into a partnership.
An Altered Self:
Living with Heart Failure

An Altered Self: Living with Heart Failure, by Sharon Bray, EdD
Eighteen years is a long time to live with any diagnosis, but especially one that quietly reshapes both the body and the mind. When I was first told I had heart failure at the age of 63, I understood it in practical, almost mechanical terms: a weakened pump, reduced efficiency, medications to compensate. What I did not anticipate—what no chart or clinical explanation fully conveyed—was how profoundly the condition would reverberate through my emotional life and sense of self, even as my cognitive abilities remained largely intact.
Once, cognition and emotion were considered separate, but we now know the two are intertwined: our emotional processes inform our cognitive ones. And for me, the greatest impact of living with heart failure has been emotional.
At 81, I continue to teach and write. I prepare lectures, organize ideas, and engage in the kind of intellectual work that demands clarity and focus. In some ways, cognitive faculties feel like old, well-used instruments—not quite as quick to tune, yet still producing meaningful output. Research on heart failure more often highlights the risk of cognitive decline, the impact of reduced cardiac output, which affects cerebral blood flow. While I’ve read these findings with interest, it’s as though they describe a life I cannot identify with.
My cognitive changes have been subtle—an occasional lapse in recall, a momentary hesitation for a word, or a need for better organization. These small shifts are also consistent with aging, but have not prevented me from sustaining the intellectual identity that has defined my life.
It is my emotional landscape that has been transformed in ways hard to quantify or explain.
Heart failure introduced a constant undercurrent of fragility in my daily life quiet awareness affecting decisions I make daily: how much energy a task requires or how I manage or interpret periods of fatigue. I am more attuned to my body in a way that, although necessary, can challenge my sense of self. I am not quite the person I once was, but rather someone who now negotiates her life with physical limitations.
Even when one remains as active as I continue to do, there are boundaries that I can no longer ignore, and they are more apparent over time. Energy is budgeted; the future is more conditional, and emotional equilibrium and self-concept are altered. I live with a persistent quiet grief, knowing my body no longer offers the same assurances it once did. Heart failure is synonymous with a persistent shift in self-concept.
Perhaps the most significant impact I’ve felt has been a gradual reshaping of self. I have had to redefine what it means to be capable, independent, and productive. I’ve had to learn to rely on my spouse more than I used to. The identity I once took for granted—energetic, independent and physically active– has been forced to include uncertainty, limitation, and adaptation. This isn’t a sudden “Aha!” moment of realization, but an ongoing process, continuing even now.
Heart failure has reframed my sense of time. When I was younger, time felt expansive, almost abstract. Now, it feels more immediate, more tangible. This is not solely a consequence of age; it’s also about living with a condition that invites reflection on mortality. Even the term “heart failure” invites thoughts of mortality. I have to work to ensure that being a heart failure patient does not diminish my engagement with life, despite limitations I once did not possess.
I seek activities that give me energy, mental challenges and, not unimportantly, fun. Writing daily, as I have done for decades, continues to be an important activity. I rely on the Japanese wisdom of “Kokoro”, or “strong hands, strong mind,” even though writing is not considered manual labour!
The emotional impact of heart failure has sharpened my awareness of what matters and, perhaps more importantly, what does not. I have less patience for trivial concerns or busy-ness for the sake of busy-ness.
At the same time, there are moments when the fear or anxiety of heart failure surfaces: a night of restless sleep, an unexpected weekend in hospital when a new defibrillator failed, or any worsening blood test results on my regular medical appointments. These feelings are not constant, but they are part of the landscape.
What strikes me, looking back over these eighteen years, is the asymmetry between the cognitive and emotional effects. While my mind has remained largely steady, the emotional part–my sense of self–has been continually reshaped in ways not always visible to others. These are not things emphasized in clinical discussions, which tend to focus on measurable outcomes. Yet I hold some responsibility for not introducing them into the conversations with my cardiologist. Nonetheless, I believe the emotional aspects in concert with the clinical ones, heart and central to understanding the lived experience of heart failure.
If there is a lesson in this, it may be that the impact of illness cannot be fully captured by cognitive tests or physiological metrics. The emotional dimension—how one feels, adapts, and finds meaning, and, not unimportantly, how one comes to understand an altered self—plays an equally important role.
Yet I would not describe these changes solely in terms of loss. There has also been continuity, resilience, and even a certain quiet enrichment. The ability to continue teaching and writing is, of course, a source of satisfaction, but there is a deeper sense of living with something difficult and still living as fully as I can.
Heart failure, as I have experienced it, is not just a medical condition. It is an ongoing negotiation between body and mind, between limitation and possibility, and between who I was and who I have become. It has asked more of me emotionally than cognitively and has reshaped my sense of self in ways that are both challenging and, at times, unexpectedly illuminating.
At 81, I do not take this lightly. Nor do I take for granted the capacity to reflect on it, to give it form in words, and to continue participating in the intellectual life that has long defined me. If the heart has faltered, the mind—and, in many ways, the spirit—has remained engaged. And perhaps that, in the end, is the most important balance I have been able to maintain.

Getting Support
Patient Support
Getting Support
Caregiver Support


Getting Support
The Ontario Caregiver Organization
Research and Study
Canadian Stroke Best Practice Recommendations:
Vascular Cognitive Impairment
The Canadian Stroke Best Practice Recommendations now include new guidance on vascular cognitive impairment (VCI), a condition that can affect memory, thinking, and attention due to problems with blood flow to the brain. This can happen after a stroke or alongside heart conditions such as atrial fibrillation or heart failure.
These recommendations were created by healthcare experts working closely with people who have lived experience of VCI, ensuring real experiences shaped the guidance. The recommendations cover the full journey of care, from recognizing early signs and getting the right tests, to treatment options, rehabilitation, prevention of further problems, and end-of-life care. A key feature is a VCI journey map, designed by people living with VCI, which shows what individuals and families may experience over time. This map helps patients, caregivers, and healthcare teams better understand needs, expectations, and supports at each stage.
This work emphasizes the importance of team-based, coordinated care that looks at both brain and heart health together. It also highlights the need for continued research to improve diagnosis, care, and quality of life for people living with VCI.
UNEARTH CVD
A large national team called UNEARTH CVD, led by Dr. Douglas Lee and Dr. Gustavo Saposnik, as well as collaborators from neurology, cardiology, psychiatry, and data science, is studying how the heart and brain interact and looking for ways to identify early signs of cognitive changes before symptoms appear. Recently, this team published the first study testing a fully digital cognitive assessment in people with heart failure, showing promise for easier and more accessible ways to check thinking skills alongside heart care. This growing research highlights how heart failure affects more than just the heart and aims to improve diagnosis and support for cognitive health as part of comprehensive care.
Research and Study
Participate in Research
Participating in research is one way people living with heart failure and cognitive changes can help improve care for themselves and others. By sharing your experiences or taking part in a study, you help researchers better understand what matters most in everyday life and care. Current studies looking for participants are listed on our Studies in Recruitment page.

Partners & Acknowledgements
This Project has been made possible by the Canada Brain Research Fund (CBRF), an innovative arrangement between the Government of Canada (through Health Canada) and Brain Canada Foundation, and Heart and Stroke Foundation of Canada. To date, Health Canada has invested over $130 million through the CBRF which has been matched by Brain Canada Foundation and its donors and partners. The views expressed herein do not necessarily represent the views of the Minister of Health or the Government of Canada.
