How is Cardiotoxicity Diagnosed and Managed?
Oncology and cardiology teams can work closely together on providing care for people undergoing cancer treatment before problems arise.
These “cardio-oncology” teams monitor patients at risk of developing heart problems during cancer therapy, diagnose any heart issues, and begin early treatment. These teams continue to monitor patients in the months and years following cancer treatment. Cardiotoxicity is diagnosed by physical exams and specific tests.
One of the goals of a cardio-oncology team is to minimize interruptions to cancer therapy, as delays and interruptions can impact long-term outcomes. By diagnosing cardiotoxicity early, the cardiology team can start medications to stabilize and improve heart function, often while the oncology team continues to administer cancer therapy.
Your cardio-oncology team is readily accessible to optimize your cardiac medications and care needs. These medications may include beta blockers, ace inhibitors/angiotensin II receptor blockers, and statins.
By self-monitoring and self-managing, patients can also help manage cardiotoxicity.
Monitoring Blood Pressure
High blood pressure is diagnosed by self-monitoring at home as well as during clinic visits. As anxiety related to clinic appointments and testing may elevate your blood pressure, at-home testing helps your team determine what your blood pressure is like in your everyday environment and can make an impact on your treatment. It is recommended that you monitor your blood pressure once a week and take those readings to clinic appointments. We strive for a blood pressure at home of less than 130/80 mm Hg.
If your blood pressure is consistently high, you may need medications to control your blood pressure. Blood pressure can be controlled with one or more medications. It can be difficult to predict how long you will have to be on blood pressure medication. Sometimes, high blood pressure is related to your specific cancer treatment and may go back to normal after your treatment is completed. However, sometimes blood pressure medication may be needed in the long-term.
Commonly used medications for high blood pressure include:
- ACE inhibitors (Ramipril, Perindopril, Lisinopril)
- Angiotension II receptor blockers (Candesartan, Valsartan, Irbesartan, Telmisartan)
- Calcium channel blockers (Amlodipine, Diltiazem)
- Diuretics (Furosemide, Hydrochlorothiazide, Chlorthalidone).
Monitoring Heart Rhythm
Abnormal heart rhythms (arrhythmias) can be detected by electrocardiograms (ECG) and Holter monitors. Sometimes patients can feel a fast or irregular heartbeat or skipped beats – these are called palpitations. Testing determines whether these palpitations are significant and require treatment.
Not all arrhythmias require treatment. Discuss with your health care provider whether medications can control the arrhythmia and prevent blood clots. These medications may include:
- Beta blockers
- Digoxin
- Anti-arrhythmic medications (amiodarone)
- Aspirin
- Anti-coagulants (blood thinners such as apixaban or coumadin).
Monitoring Troponin Levels
Troponin is a heart protein not normally found in the blood. However, it is released into the bloodstream when the heart is injured. The greater the damage to the heart, the higher the level of troponin in the blood. For example, patients who have had heart attacks typically have high levels of troponin in their blood at the time of their injury.
Patients at risk for heart injury during their cancer therapy may have troponin levels checked during their treatment. This allows health care providers to detect heart injury before the onset of heart failure symptoms.
Treating Coronary Artery Disease
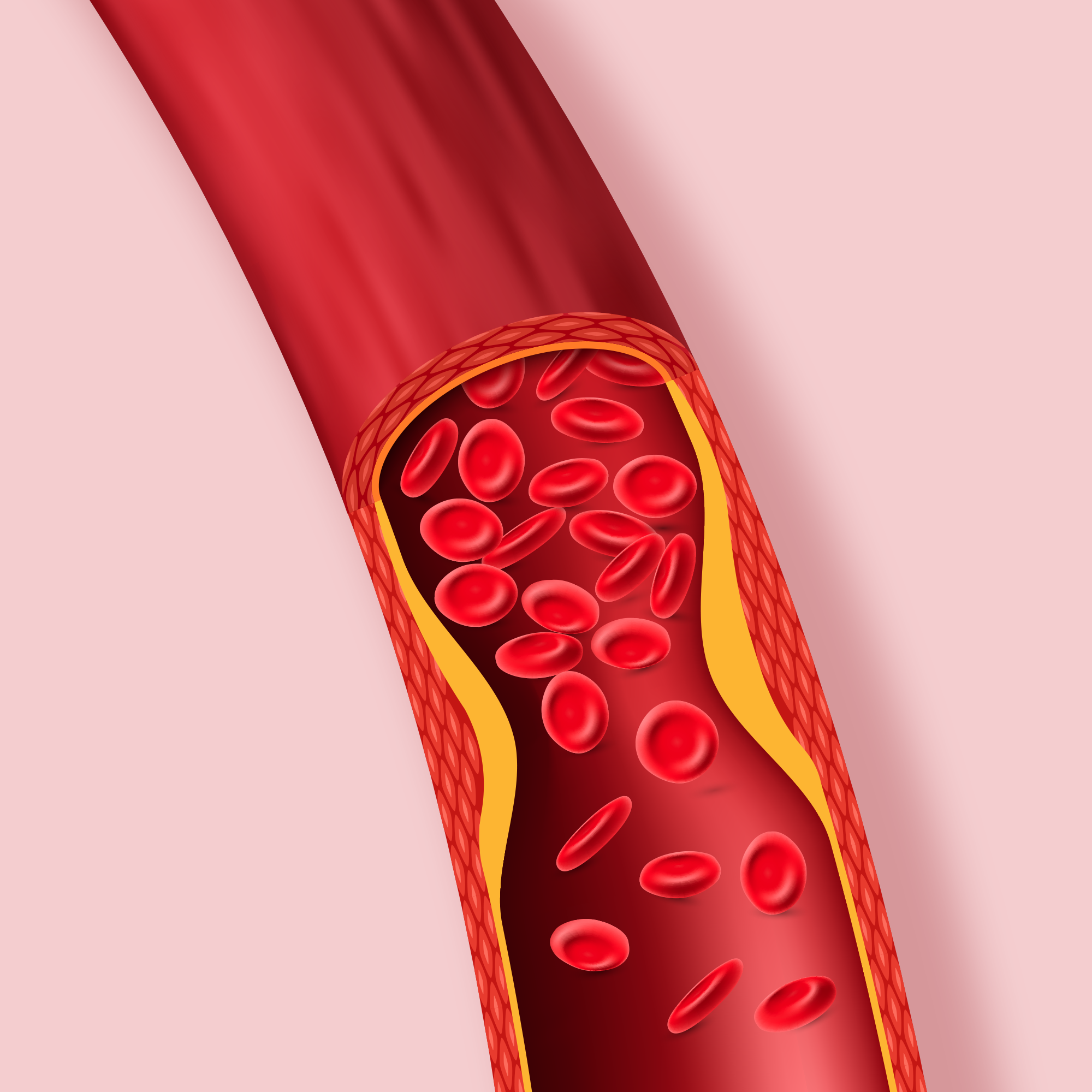
Narrowing and thickening of the arteries of the heart is caused by cholesterol deposits, which leads to coronary artery disease (CAD). While this typically takes years, some cancer therapies can increase the rate of this process.
Coronary artery disease is treated with medication and may require a coronary angiogram (a dye test to look for narrowing of arteries) and stenting or bypass surgery.
Learn more about coronary artery disease diagnosis and treatment.
Treating Coronary Artery Vasospasms
- Chest pain or sudden shortness of breath shortly after receiving chemotherapy/immune therapy
- Chest pain that is not relieved with nitroglycerin
- Chest pain that includes dizziness, fast heart rate, or sweating
Treating Myocarditis
Myocarditis is an inflammation of the heart muscle. It can be related to viral infections or may be a side effect of cancer therapies.

 Sharon Bray
Sharon Bray
 Paula Henderson
Paula Henderson
 Isabel Victal
Isabel Victal
 Cindy
Cindy