What is Heart Failure?
Heart failure describes a condition where the heart is unable to meet the needs of the body. It is a chronic condition, which means most people live with heart failure for the rest of their lives and will eventually die from it.
Heart failure is very common. Currently, more than 750,000 Canadians are living with heart failure, with 100,000 people diagnosed with the condition every year. It is one of the leading causes of hospitalization in Canada.
Heart failure usually affects people later in life but can occur at any age. With the aging population and enhanced detection tools, the number of people diagnosed with heart failure is expected to grow significantly.
While a diagnosis of heart failure sounds frightening, it does not mean that your heart is going to stop in the near future or that you are going to die soon. Advances in care and treatments continue to help patients live longer and improve quality of life.
What are Heart Failure Symptoms?
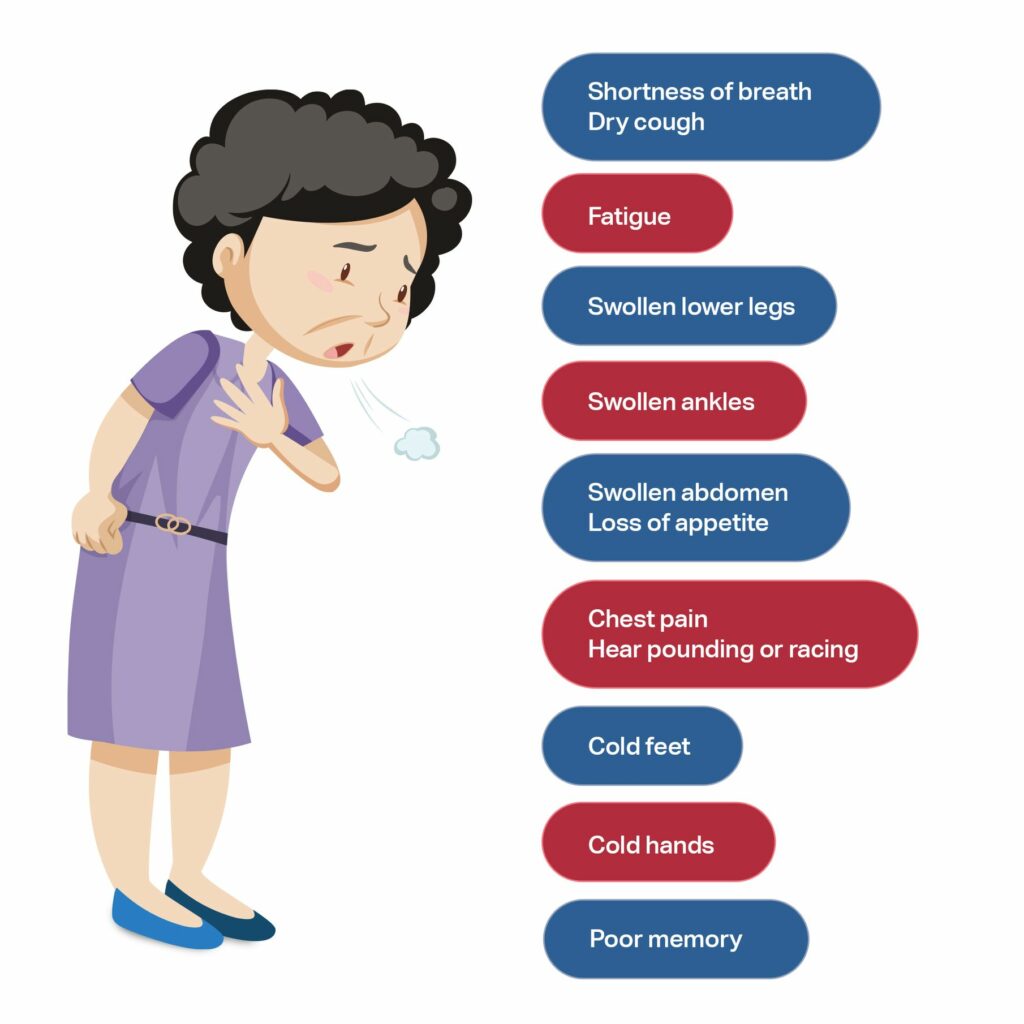
The main symptoms of heart failure are fatigue, shortness of breath, and swelling in the lower legs, ankles and/or abdomen. These symptoms may come and go or occur at the same time.
Many patients with heart failure tend to retain fluid. Fluid can accumulate in the legs, causing swelling; in the abdomen, causing bloating and poor appetite; and in the lungs, causing shortness of breath. When someone with heart failure retains too much fluid, their symptoms worsen, and they may require admission to hospital for further treatment.
Other symptoms of heart failure may include:
- Poor memory and difficulty concentrating
- Cold hands and feet
- Shortness of breath when lying flat, and having to use many pillows to be comfortable
- Waking up at night feeling short of breath
- Waking up at night to urinate
- Dry cough, which may be worse when lying flat
- Loss of appetite or feeling full quickly after eating small amounts
- Chest pain
- Feeling the heart pound or beat quickly
Not every patient with heart failure will experience all these symptoms.
As well, many of these symptoms can be caused by conditions other than heart failure. If you are not sure if a symptom you are experiencing is related to heart failure, speak to your health care professional.
How Severe is Heart Failure?
Heart failure is a progressive condition. However, the course of illness is highly variable between patients, and it is often only diagnosed once symptoms develop, and patients seek medical attention.
Prior to the onset of any symptoms, individuals may have developed changes to the structure and function of their heart.
There are several factors that healthcare providers take into consideration to help assess the degree of heart failure:
- Size of the heart
- Pumping function of the heart (sometimes referred to as ‘ejection fraction’)
- Heart valve function
- Kidney function
- Blood tests measuring injury and strain on the heart.
However, the most important measure of heart failure severity is the degree to which patients experience symptoms.
Patients who experience only mild symptoms with minimal impact on their day-to-day function are considered to have less severe heart failure. In contrast, patients with very poor function and high symptom burden are often unable to carry out ordinary activities.
If heart failure symptoms become severe, the prognosis is less favorable, and patients may require frequent visits to the emergency department or recurrent admissions to hospital to manage the effects of severe or ‘advanced’ heart failure.
How is Heart Failure Classified?
One system to assess the severity of a patient’s heart failure is the New York Heart Association (NYHA) Functional Classification that relates symptoms to everyday activities and quality of life:
- Class I symptoms: No limitations due to heart failure. Patients generally feel well.
- Class II symptoms: Mild limitation due to heart failure. Symptoms can occur with ordinary activity.
- Class III symptoms: Moderate limitation due to heart failure. Symptoms occur with less than ordinary activity.
- Class IV symptoms: Severe limitation due to heart failure. Symptoms are worsened with any type of activity.
For all people with heart failure, lifestyle changes, medications, and other treatments aim to minimize symptoms and keep people well enough to manage their condition and avoid hospitalization.
What Causes Heart Failure?
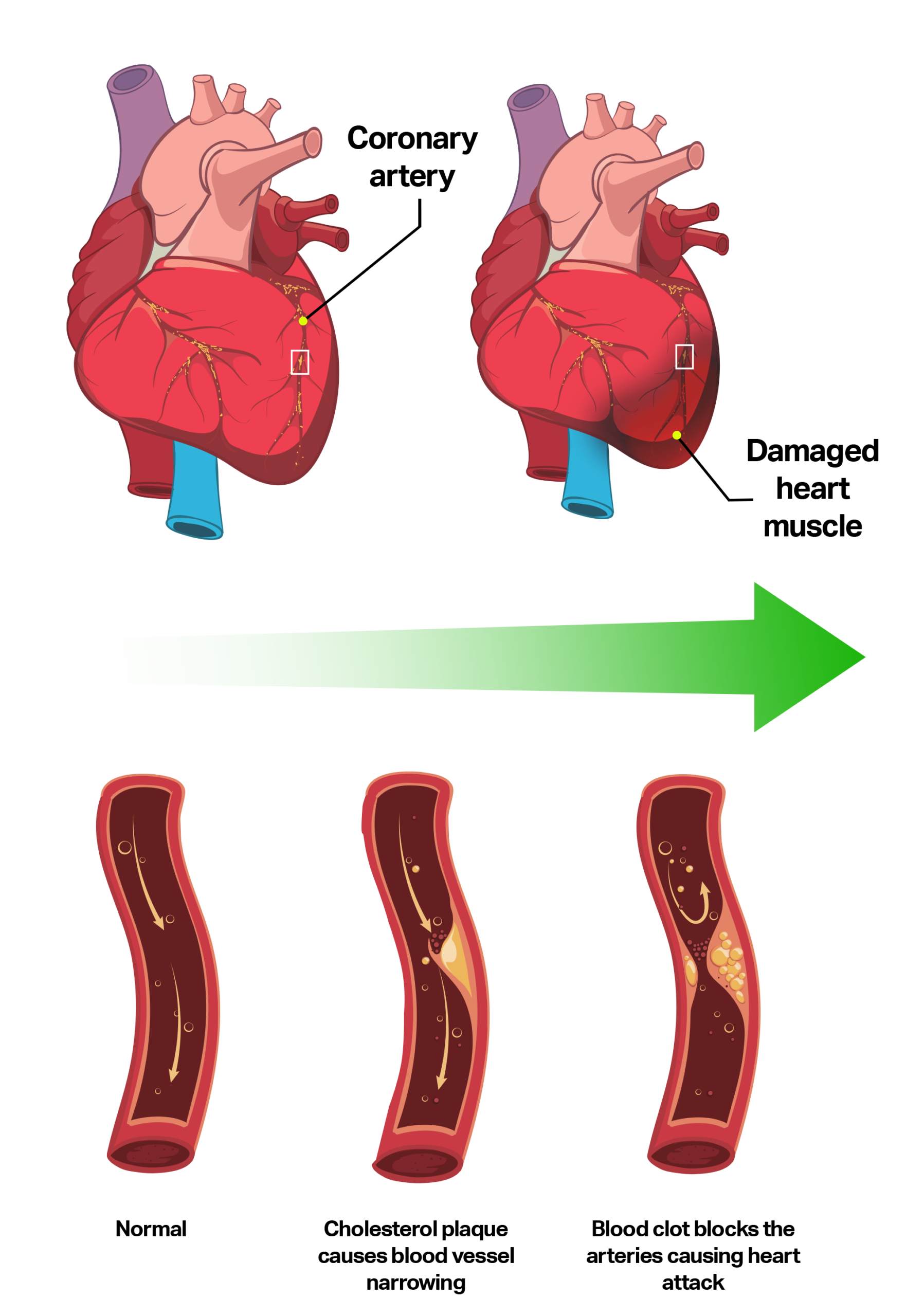
Coronary Artery Disease
The most common cause of heart failure in Canada is coronary artery disease. This is the accumulation of cholesterol plaque within artery walls. If cholesterol plaque occurs over an extended period, it can lead to chronic narrowing in the arteries, restricting the flow of blood and oxygen to the heart muscle.
When coronary artery disease is the cause of a weakened heart muscle, the condition is called ischemic cardiomyopathy (ischemic = lack of blood flow, and cardiomyopathy = heart muscle problem).
More acutely, a heart attack can happen when a cholesterol plaque in the wall of an artery ruptures open and causes a blood clot to form, immediately blocking the arteries and starving the heart muscle of blood and oxygen. It is difficult to tell which cholesterol plaques are at risk of rupturing and causing a heart attack.
When a large area of heart muscle is damaged or affected by coronary artery disease or a heart attack, the heart may become weak. This can lead to heart failure. It is not always clear why some patients with a damaged or weakened heart will develop heart failure while others will not.
It is important to know if coronary artery disease has caused a weakened heart muscle, because if the blocked arteries can be opened (either with stents or bypass surgery), heart function may improve.
Other Causes of Heart Failure
There are many other causes of heart failure. These include:
- Long standing high blood pressure
- Diabetes
- Heart valve problems (leaky or tight valves)
- Abnormal heart rhythms (called arrhythmias)
- Toxins (like excessive alcohol or certain chemotherapies)
- Viral infections that affect the heart
- Congenital heart conditions
- Genetic (inherited) conditions.
Types of Heart Failure
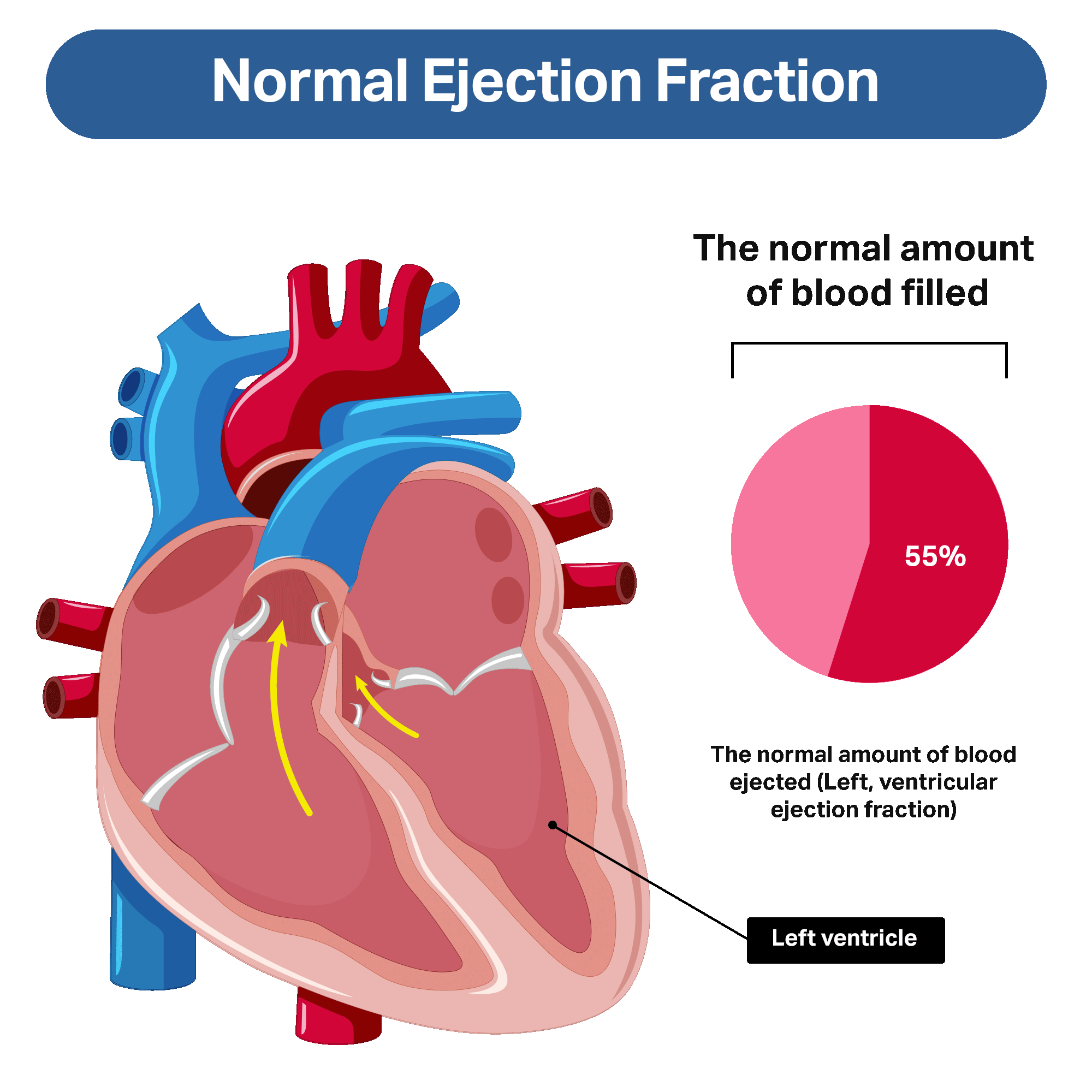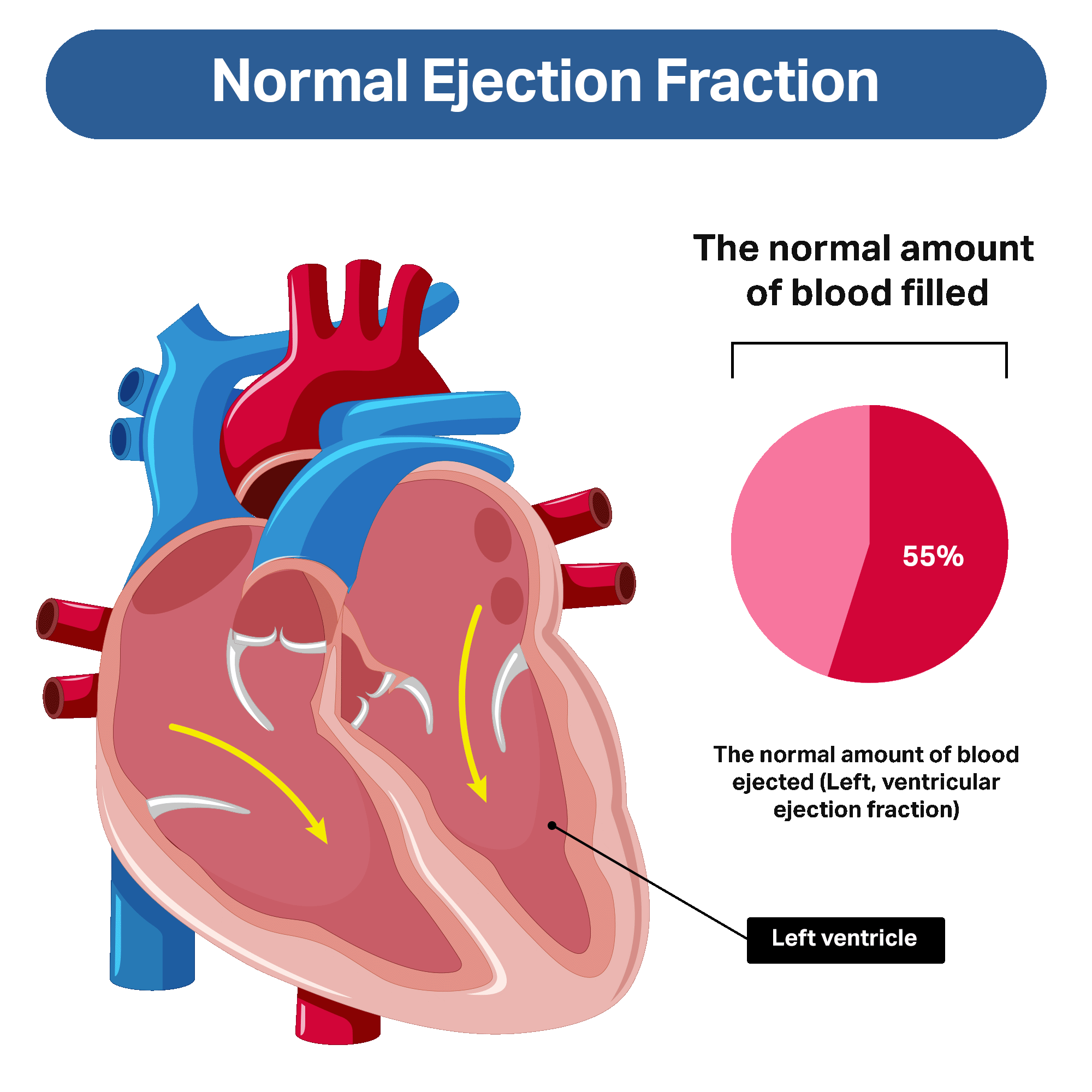
There are many ways to classify heart failure. Heart failure is commonly described according to the left ventricular ejection fraction (or EF).
The left ventricular ejection fraction refers to the amount of blood that is “ejected,” or pumped out, with each heartbeat. A normal ejection fraction is not 100%, as the heart does not completely empty with blood with every heartbeat. Instead, a normal ejection fraction is about 55% or more.
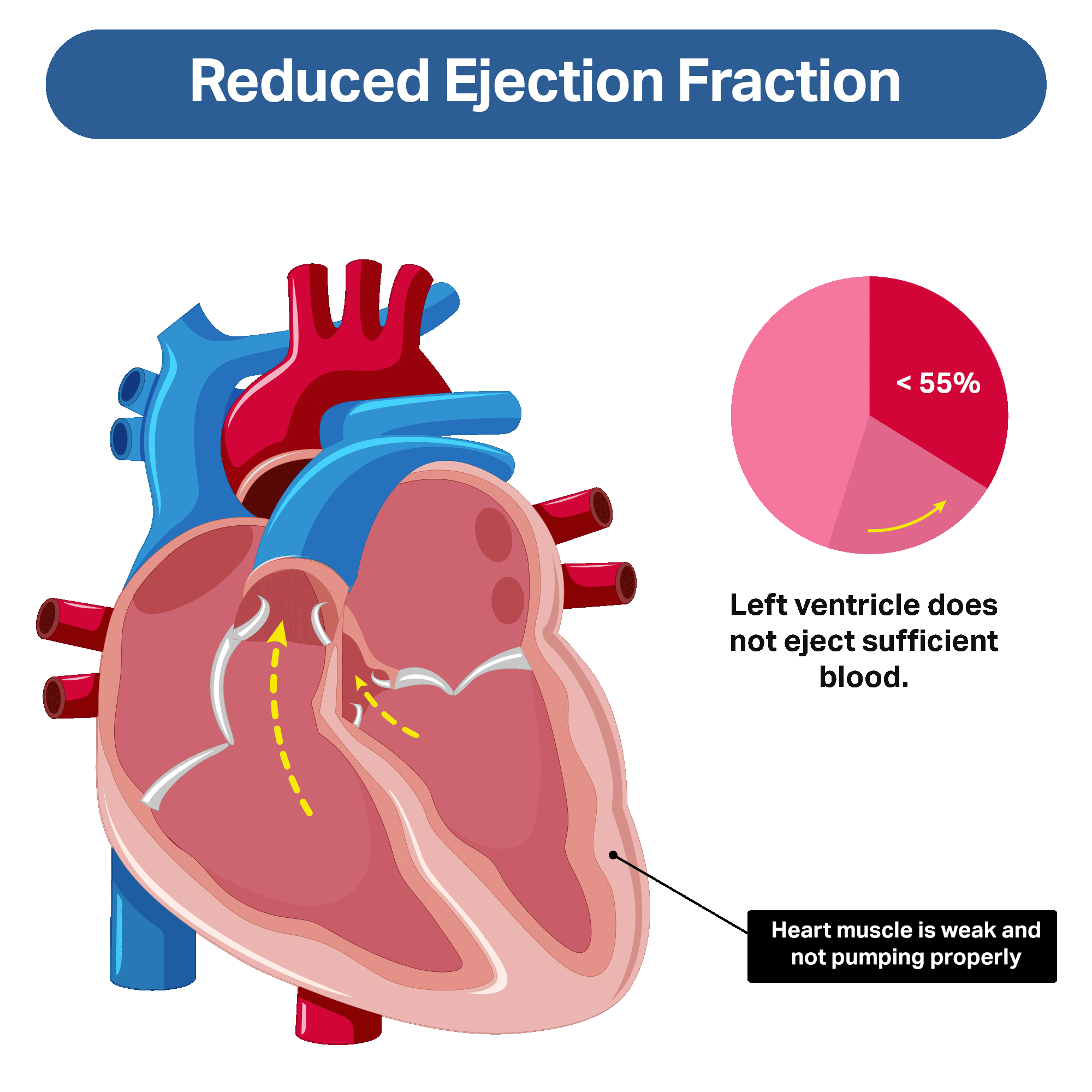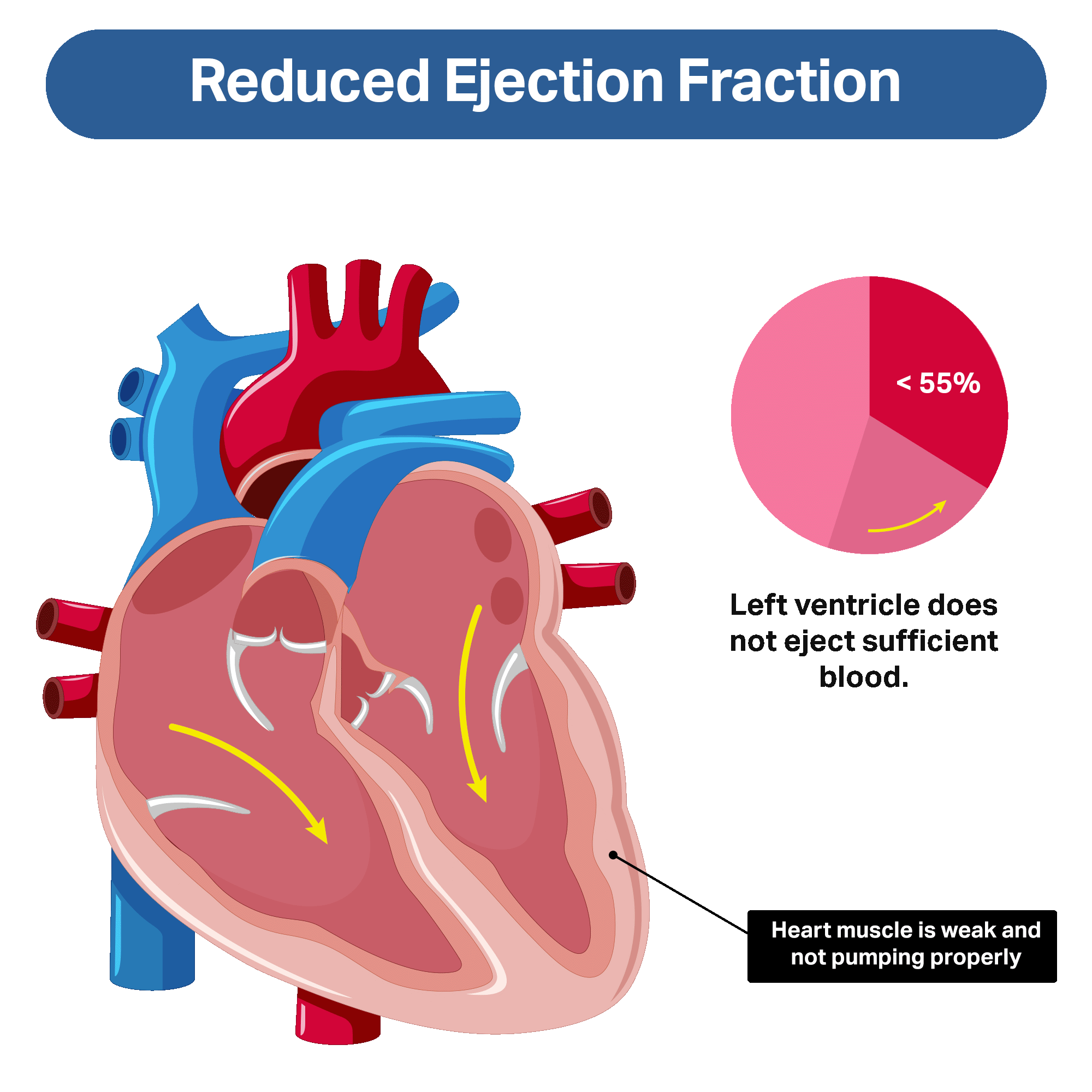
Two types of heart failure are described according to EF: low (or “reduced”) ejection fraction, or normal (or “non-reduced”) ejection fraction.
In people with reduced ejection fraction, the problem is primarily with the pumping function of the left ventricle. The left ventricle is weak and doesn’t eject a sufficient amount of blood during each heartbeat.
The acronym is HFrEF (pronounced Hef-ref). You may see this in your chart or on your test results.
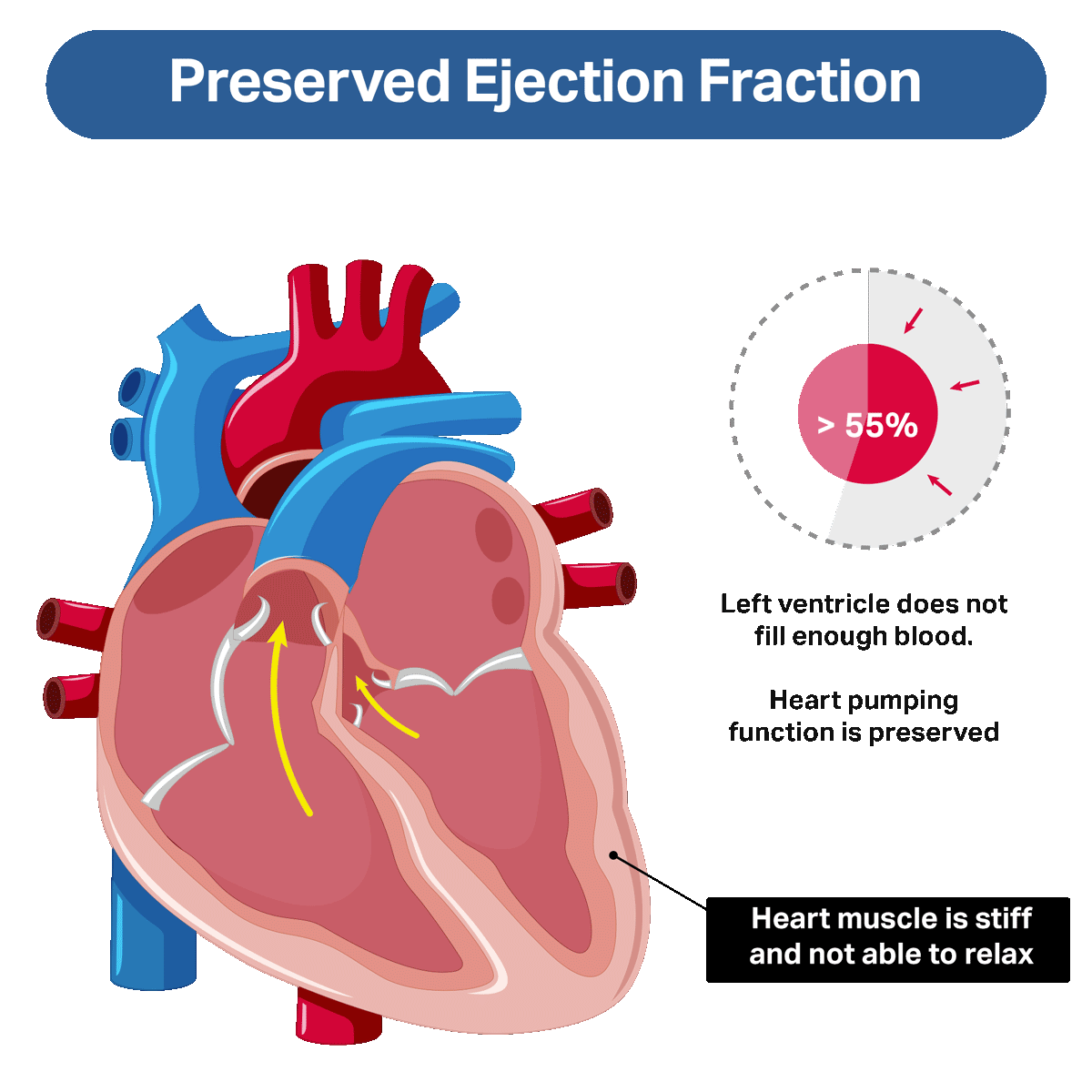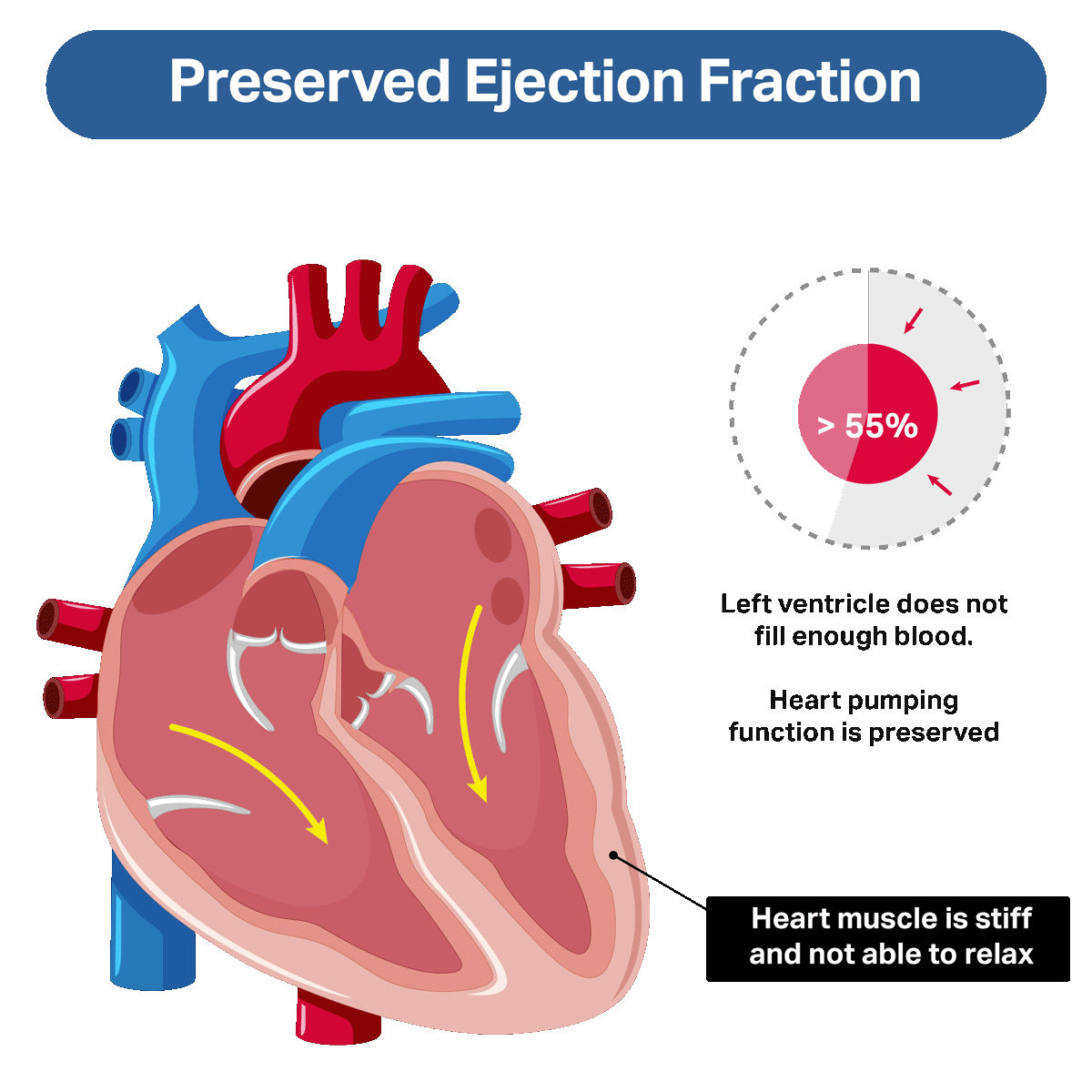
The pumping function of the heart is normal in people with non-reduced ejection fraction, but the problem is the heart’s inability to relax properly. This reduces the volume of blood able to fill the left ventricle during the diastolic, or filling, phase of each heartbeat.
The acronym is HFnrEF (pronounced Hef-non-Ref). You may see this in your chart or on your test results. HFnrEF was previously called “preserved” ejection fraction (HFpEF). You may still hear some people refer to it in this way.
Both types of heart failure result in the same symptoms – fatigue, shortness of breath, and swelling.
If the ejection fraction is reduced or non-reduced, it determines treatment options. will differ accordingly. An echocardiogram (ECHO) is usually performed to determine whether the ejection fraction is reduced or non-reduced.
Therapies (medications, devices) that have been shown to make people live longer with heart failure apply mainly to people with reduced ejection fraction. The management of heart failure with non-reduced ejection fraction focuses mainly on controlling an individual’s risk factors (high blood pressure and diabetes) and making sure they don’t retain extra fluid. This is an area of active research, and recent studies have shown great promise for some medications to improve the prognosis for patients with non-reduced ejection fraction.
What is Advanced Heart Failure?
Advanced heart failure is a term that is often used by care providers to indicate that the heart failure condition has progressed and has become more severe. Patients may even be referred to an “advanced heart failure specialist” to be assessed for specialized interventions aimed at improving life expectancy and overall quality of life.
Therapies for advanced heart failure include heart transplantation, long-term ventricular assist devices, long-term intravenous diuretic therapy, some forms of dialysis and palliative medical therapy.
There is no single or universal definition of ‘advanced heart failure.’ In general, this state is associated with different markers or signs of deteriorating health and worsening prognosis. Some characteristics of advanced heart failure typically include:
- Multiple hospital admissions for heart failure in the past year
- Severe limitation of daily activities due to heavy symptom burden, usually including significant fatigue and shortness of breath
- Difficulty controlling fluid build-up (edema) with increasing diuretic requirements
- Difficulty tolerating medications because of low blood pressure or worsening kidney function
- Increasing number of shocks from an Implantable Cardioverter Defibrillator (ICD)
- Abnormal bloodwork indicating worsening strain on the heart (rising BNP levels or troponin levels) or worsening organ function (rising creatinine or liver function tests, low sodium levels)
- Progressively worsening heart function or elevated pressures in the heart and lungs as indicated by an ECG
- Poor performance on formal exercise testing

 Sharon Bray
Sharon Bray
 Paula Henderson
Paula Henderson
 Isabel Victal
Isabel Victal
 Cindy
Cindy